Hospice Acronym Alphabet Soup
Are you confused by the Acronym Alphabet Soup?
Does the never ending list of acronyms used in the hospice and healthcare industry leave you confused?
Are you worried that you may confuse CMN with CMP?
To help sort out the confusion, we add here links to lists of acronyms:
- Acronyms commonly found on the cms.hhs.gov website as well as other acronyms commonly used in hospice and healthcare: Acronyms – from CMS
- A hospice quality reporting acronym list: Acronyms – from HQRP
- NHPCO acronym listing: NHPCO acronyms
Use these acronym listings to help clarify things when you inevitably are faced with acronym confusion!


Timely filing of Notice of Election
The Notice of Election (NOE) is more than a clinical administrative task; it is a critical financial trigger. In the hospice revenue cycle, the NOE serves as the formal notification to Medicare that an agency has assumed responsibility for a patient’s care. Failure to file this document within the mandatory window results in permanent, unrecoverable revenue loss.
The Standard for Timely Filing
Medicare regulations require that an NOE be filed within five calendar days after the beneficiary’s hospice admission date. For a filing to be considered legally “timely,” it must meet two specific criteria:
- Receipt Date: The NOE must be received by the Medicare contractor within five calendar days after the admission date.
- Processing Status: The NOE must successfully process and reach the final status/location P B9997.
The Cost of Non-Compliance
When an NOE is filed late, the financial consequences are immediate. Medicare will not reimburse the agency for the days of care provided from the date of admission until the date the NOE is finally submitted and accepted.
Consider this example of a late filing:
- Admission Date: May 1st
- NOE Receipt Date: May 10th
- The Result: The agency is responsible for the cost of care from May 1st through May 9th. These nine days are considered “non-covered” and represent a 100% loss of revenue for that period.
The “RTP” Trap: Resubmissions and Timeliness
One of the most common drivers of revenue loss is the Return to Provider (RTP) error. If an NOE is submitted within the five-day window but contains errors, it will be sent back for corrections.
It is critical to understand that the resubmission date becomes the new “receipt date” for timeliness purposes. Even if your initial attempt was on day two, if the corrected version isn’t accepted until day ten, the entire period remains non-covered. This is why “clean” initial submissions are just as important as “fast” submissions.
Operational Requirements for Late Filings
If an agency identifies that an NOE was filed untimely, the subsequent claim must be coded specifically to reflect the non-covered period. This is not optional; failure to code correctly can lead to claim rejections or audits.
- Occurrence Span Code (OSC) 77: This must be used on the claim to identify the specific dates that are non-covered due to the late NOE.
- Dual-Line Billing: The claim must be split into two distinct rows: one for the non-covered days (associated with OSC 77) and one for the covered days following the NOE acceptance.
Leadership Strategy: Moving to a 48-Hour Standard
To eliminate the risk of late filings, high-performing agencies do not aim for the five-day deadline. Instead, they implement an internal 48-hour submission rule.
By requiring NOEs to be filed within two days of admission, leadership creates a “buffer” to handle unexpected RTP errors or technical issues with the billing software. This proactive operating rhythm ensures that administrative delays never compromise the agency’s financial stability or the clinical team’s ability to focus on patient care.
What is a MAC?
A Medicare Administrative Contractor (MAC) is a private health care insurer that has been awarded a geographic jurisdiction to process Medicare Part A and Part B medical claims for Fee For Service (FFS) beneficiaries.
CMS relies on these contractors to serve as the primary operational contact between the Medicare FFS program and the health providers enrolled in the program.
MACs are multi-state regional contractors who are responsible for administering Part A and Part B claims.
What types of MACs are there?
There are two types of MACs: Part A/B MACs and DME MACs.
Hospice claims are administered by Part A/B MACs. Part A/B MACs process about 95% of all FFS claims.
There are 12 Part A/B MACs.
Four of the MACs specialize in processing claims for hospice and home health providers
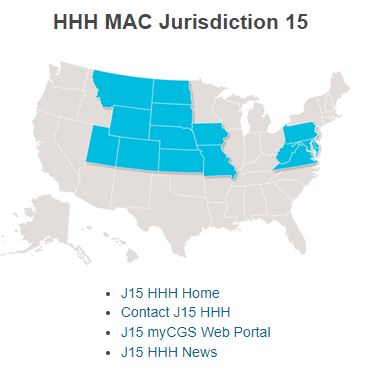
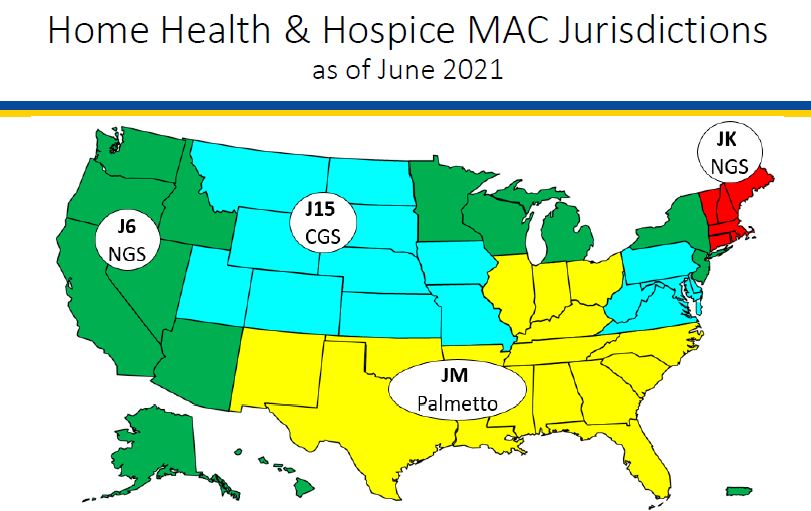
What geographic areas do each of the hospice and home health MACs cover?
The following map shows the geographic regions that each of the hospice MACs is responsible for administering.
What activities do MACs perform?
MACS perform a number of activities including:
- Provider Enrollment
- Claims processing, payment, and payment notices
- Provider customer service (but not beneficiary customer service)
- Audit provider cost reports
- Respond to provider inquiries
- Audit payments and review medical records
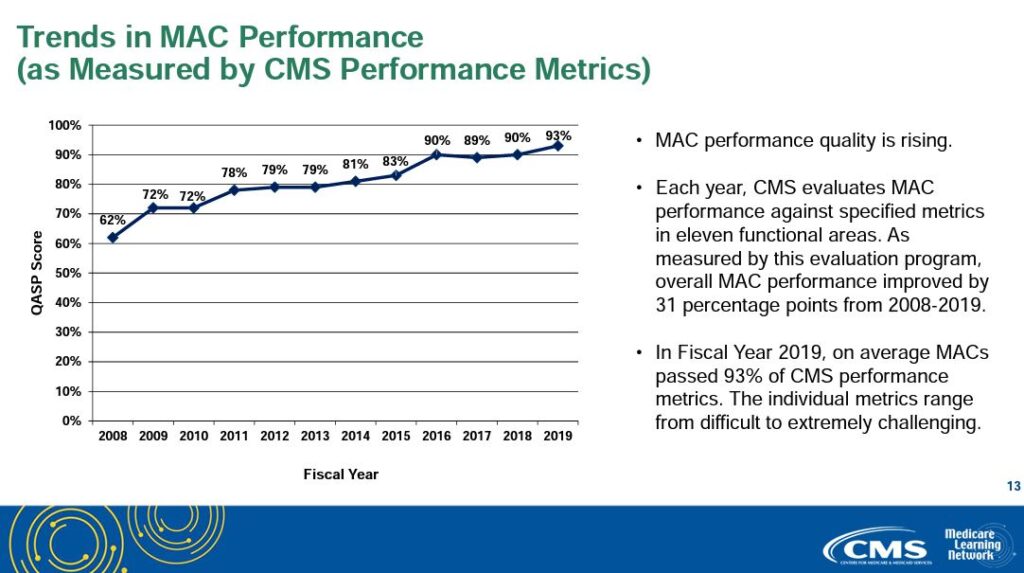
How are MACs measured and how well do they perform?
Each year, CMS evaluates MAC performance against specific metrics in eleven functional areas. MAC performance quality has been consistently improving since CMS began measuring MAC performance. Average MAC performance has increased from 62% to 93% since CMS began measuring MAC performance.
Print ‘n take hospice keys
- Seeking to contact your MAC? Here’s their contact information
hospiceKeys - CMS MAC contact
Download
- A map of MAC regional jurisdictions
hospiceKeys - CMS MAC
Download
Where can you find more information?
This PowerPoint from Medicare Learning Network provides more helpful information about MACs: MLN MAC PowerPoint

How to Submit a Notice of Election (NOE)
What is a Notice of Election?
When a Medicare beneficiary elects hospice services, the hospice must complete an election notice with the beneficiary and file a Notice of Election (NOE) with Medicare. A Notice of Election (NOE) is the formal mechanism used to notify Medicare that a beneficiary has elected the hospice benefit. While the concept is straightforward, the submission process requires high technical accuracy to meet the mandatory five-day filing window.
Submission Timing and the “Clean Claim” Requirement
Medicare requires that an NOE be submitted and processed before the agency files its first claim for that beneficiary. Since October 1, 2014, the standard has been strict: the NOE must be filed within five calendar days of the election date.
To satisfy this requirement, the submission must be “clean” – meaning, it is free of data entry errors. If an NOE contains errors, it is Returned to Provider (RTP). Once corrected and resubmitted, the NOE receives a new receipt date, which can push the filing outside the five-day window and result in non-covered days.
Three Methods for NOE Submission
Hospice providers currently have three avenues for submitting the NOE. Each carries different levels of administrative burden and risk of error.
1. Electronic Data Interchange (EDI) – Recommended
Effective January 1, 2018, Medicare allowed for NOE submission via EDI. This is the most efficient method for agencies seeking a predictable operating rhythm.
- The Benefit: Data is exported directly from the patient’s Electronic Medical Record (EMR), virtually eliminating manual keying errors.
- Operational Note: NOEs submitted via EDI should not be batched with standard claims; they must be processed as distinct transactions.
2. Direct Data Entry (DDE)
DDE involves manually entering the NOE into the Fiscal Intermediary Shared System (FISS).
- The Benefit: DDE provides real-time access to monitor claim status, check beneficiary eligibility, and correct errors.
- The Risk: Because this requires manual entry across multiple screens, it is highly susceptible to human error, which often leads to RTP status and potential filing delays.
3. Paper Submission (UB-04)
While technically permitted, submitting a physical UB-04 form via mail is the least efficient method.
- The Risk: This method is subject to mail delays and manual processing times at the Medicare Administrative Contractor (MAC), making it nearly impossible to guarantee compliance with the five-day window.
Ensuring Submission Accuracy
Regardless of the method chosen, the data requirements remain the same. Leadership should ensure that the billing team is utilizing verified “job aids” from their specific MAC (such as Palmetto GBA, CGS, or NGS) to ensure every data field – from the NPI to the admission date – is perfectly aligned with the election statement.
By prioritizing EDI submission, agencies can reduce their reliance on manual intervention and ensure that the “engine” of the revenue cycle remains stable and compliant.

Unusual Circumstances: Face to Face Encounters
Prior to the third hospice benefit period, and prior to each subsequent benefit period, a hospice physician or nurse practitioner is required to have a face to face encounter with the hospice patient to recertify that the patient continues to be Medicare eligible for hospice benefits. The face to face encounter must occur within 30 calendar days prior to the start of the third benefit period and each subsequent benefit period.
The face to face encounter is necessary to recertify that the patient remains eligible for Medicare hospice benefits. If face to face encounters are not performed timely, the patient is is no longer hospice eligible. The hospice may continue to provide hospice services to the patient but may no longer continue to bill Medicare. Instead, the hospice would need to assume all financial responsibility for the patient until such time that the hospice is able to reestablish patient hospice eligibility. The patient may be readmitted to hospice once hospice eligibility criteria are once again met.
What if there are exceptional circumstances that cause the hospice to be unable to timely complete the face to face encounter?
What are exceptional circumstances?
If a patient is admitted and is in the third benefit period or later, the hospice agency may be unable to perform the face to face encounter prior to the start of the benefit period.
For example, if the patient is an emergency weekend admission and the nurse practitioner or hospice physician is unable to meet with the patient prior to hospice admission. The patient is only seen the following Monday.
Another exceptional circumstance may be where the CMS data system is unavailable and the hospice agency is unaware that the patient is in the third or later benefit period.
In these documented exceptional circumstances, the face to face encounter is considered timely if it is completed within two days after admission.
In addition, if the patient dies within two days of admission, the face to face encounter is considered complete.
Where can you get more information?
Details on Medicare Face to Face encounter requirements: Medicare F2F encounter requirements
