
by editor | Aug 11, 2024 | Care Keys - Aides, Clinical Compliance
An incident report is a special kind of report that you write when something unusual or unexpected happens during your visit with a patient. This could be anything that isn’t part of the normal care routine.
When to Write an Incident Report
An incident report is needed if:
- The Patient Falls: If the patient slips, trips, or falls, even if they don’t seem hurt.
- An Injury Happens: If the patient, a family member, or even you get hurt in any way.
- A Medication or Care Error: If the wrong medicine is given, or if medicine is given at the wrong time or if there a different error in patient care.
- Behavior Changes: If the patient suddenly becomes very confused, angry, or upset.
- Safety Concerns: If something dangerous happens or almost happens, like if a patient tries to leave the house when they shouldn’t or if you feel uncomfortable or unsafe.
- Property Damage: If anything breaks or is damaged during the visit.
- Blood or Fluid Exposure: If you are exposed to blood or body fluids during the visit.
How to Write an Incident Report
- Write It Right Away: Write the report as soon as the incident happens. This way, the details are fresh in your mind.
- Stick to the Facts: Describe exactly what happened. Don’t guess or add your opinions. Just describe what you saw and heard.
- Be Specific: Include details like the time, place, and exactly what happened. If someone said something important, use their exact words.
- Report Injuries: If anyone was hurt, describe the injury and what was done to help.
- Include Witnesses: If someone else saw what happened, include their name and what they saw.
- Stay Calm: Use clear and simple words. Don’t blame anyone in the report, just describe what happened.
- Tell Your Supervisor: Always report the incident to your supervisor as soon as possible.
Why Incident Reports Matter
- Safety: Incident reports help keep patients and caregivers safe by making sure everyone knows about any problems or risk.
- Improvement: These reports help the care team learn from mistakes and prevent them from happening again.
- Legal Protection: Documenting incidents protects you and the agency by showing that you reported what happened.

by editor | Aug 11, 2024 | Care Keys - Aides
When you talk to a patient, you share information with them, and they share information with you. Communication can happen in many ways, such as:
- Talking
- Writing
- Pictures
- Drawing
- Actions
Understanding the Patient’s Emotions
- Empathy: Try to understand how the patient feels. Showing that you care can help build trust and make the patient feel calmer.
- Non-Verbal Communication: Pay attention to the patient’s body language, facial expressions, and actions, especially if they can’t talk.
Encouraging Communication
- Ask Simple Questions: Use simple yes/no questions or short sentences to help the patient express themselves.
- Repeat Back: To make sure you understood, repeat what the patient said in your own words.
Handling Difficult Behavior
Sometimes, patients might act in a way that seems angry or upset. They might hit, bite, push, yell, scream, or kick. Patients might do this because:
- They feel frustrated.
- They don’t feel well.
- It’s just part of their personality.
Remember, it’s not usually about you. The patient is likely reacting to how they feel. But it’s important to write down what happened and tell your supervisor. The care team needs to know about this behavior because it might show that the patient’s health is changing.
How to Respond When a Patient is Upset
- Protect Yourself: If the patient tries to hit or kick, block the blows or move out of the way. Never hit back.
- Give Them Time: Let the patient calm down before you try to talk to them again.
- Keep Them Safe: Make sure the patient is in a safe place.
- Give Them Space: Let the patient have some room and don’t crowd them.
- Stay Calm: Speak in a calm, quiet voice.
- Be Patient: Take your time and be flexible with the patient.
- Stay Neutral: Don’t argue or get into a fight with the patient. Stay calm, even if they say something mean.
- Use Gentle Movements: Don’t make sudden gestures or movements that might scare the patient.
- Be Supportive: Reassure the patient that you are there to help.
- Think About the Cause: Try to figure out what might have made the patient upset.
- Report the Behavior: Always tell your supervisor about any bad behavior so they can help.
Dealing with Non-Responsive Patients
- Gentle Encouragement: Some patients might not respond at all. Keep talking gently and offering encouragement. Even if they don’t answer, they might still hear you and feel comforted by your presence.
- Use of Familiar Items: Show the patient familiar objects like photos or favorite items. This can help them feel more at ease and might help them open up.
Involving the Family
- Family Support: Encourage family members to be part of the communication process when possible. They can often help calm the patient or provide important information about what might upset or comfort them.
Where Can You Find More Information
by editor | Aug 11, 2024 | Care Keys - Aides
Before you start taking care of a patient, follow these important steps. Doing them each time helps you remember and makes them a habit, ensuring both you and your patient are safe and comfortable.
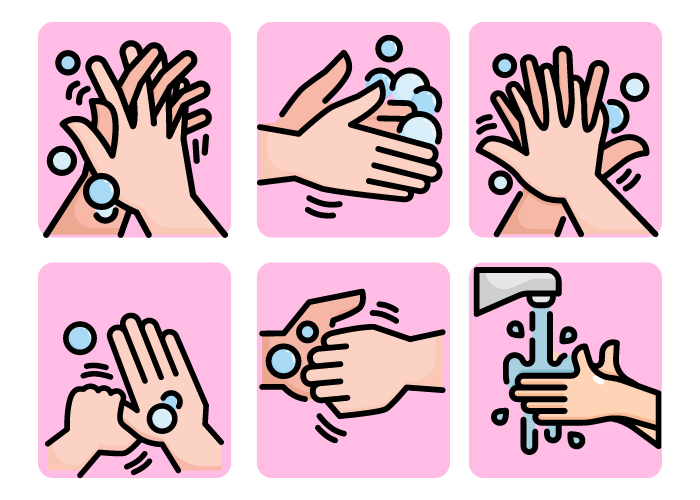
1. Wash Your Hands:
Washing your hands helps stop the spread of germs and keeps everyone healthy. Many illnesses spread if hands are not washed properly. Always wash your hands before you start taking care of a patient.
How to Wash Your Hands:
- Soap and Water: If you have soap and water, scrub your hands with soap for at least 20 seconds. Make sure to wash all parts of your hands, including between your fingers and under your nails.
- Rinse: Rinse your hands with clean, running water.
- Hand Sanitizer: If soap and water are not available, use hand sanitizer with at least 60% alcohol. Rub it all over your hands until they are dry.
Tip: You might need to wash your hands more than once during patient care. Always wash before starting any new task.
2. Explain the Procedure to the Patient and Family
Tell the patient and their family what you are going to do. This helps them feel less worried and more willing to help.
How to Communicate:
- Speak Slowly: Use simple words that are easy to understand.
- Speak Clearly: Make sure your words are clear and easy to hear.
- Eye Contact: Look at the person you are talking to. This helps build trust and ensures they are listening.
Tip: Talking calmly and clearly can help reduce anxiety and make the procedure go more smoothly.
3. Give the Patient Privacy
Make sure the patient feels comfortable and respected by giving them privacy during care.
How to Provide Privacy:
- Close Curtains or Doors: Use curtains or doors to create a private space.
- Cover the Patient: Use sheets or blankets to cover the patient as needed.
Tip: Privacy helps the patient feel more at ease and respected during care.
4. Keep the Patient Safe
Ensure the patient is safe throughout the care process.
Safety Measures for Patients
- Adjustable Bed: If the patient is in a bed that can move, lower the bed to the lowest position and lock the wheels to prevent movement.
- Wheelchair: If the patient is in a wheelchair, lock the wheels to keep the chair stable.
Tip: Regularly check that the bed and wheelchair are in the correct position and locked properly.
5. Think About Your Safety
Your safety is also important. Proper positioning and adjustments help prevent injury.
Safety Tips for Caregivers:
- Adjustable Bed: Adjust the bed to a height that is comfortable for you to avoid bending or reaching awkwardly.
- Proper positioning: Make sure you are in a good position to avoid straining your back or hurting yourself. Use proper lifting techniques.
Tip: If the bed or chair needs to be adjusted, do so before starting the procedure to make it easier and safer for you.
Additional Tips
- Routine Checks: Regularly review these steps to ensure you are following them correctly.
- Ask for Help: If you are unsure about any procedure or need assistance, ask a supervisor or colleague.
Where Can You Get More Information
CDC Hand washing protocol

by editor | Aug 11, 2024 | Care Keys - Aides
It’s important to follow these steps after you finish taking care of a patient. Doing these steps every time helps you remember them and makes them a habit. This helps keep both you and your patients safe and healthy.
1. Lower the Patient’s Bed
If you raised the bed to take care of the patient, be sure to lower it back down to its lowest position. This helps prevent falls and keeps the patient safe.
Tip: Always check that the bed is locked in place after lowering it.
2. Wash Your Hands
Washing your hands stops the spread of germs and helps keep everyone healthy. Always wash your hands after finishing any patient care.
How to Wash Your Hands:
- Soap and Water: Scrub your hands with soap for at least 20 seconds. Make sure to wash all parts of your hands, including between your fingers and under your nails.
- Rinse: Rinse your hands with clean, running water.
- Hand Sanitizer: If soap and water aren’t available, use hand sanitizer with at least 60% alcohol. Rub it all over your hands until they are dry.
3. Write Down What You Did
Take notes about the care you provided, how the patient is doing, and any important information about the family or caregiver. Writing down what you did helps ensure the patient gets the best care.
Why It’s Important:
- Communication: Your notes help the healthcare team understand the patient’s condition and decide if any changes are needed in their care.
- Quality of Care: Detailed notes ensure the patient receives consistent and high-quality care.
- Legal Requirement: Accurate documentation is required by law. If you don’t record what you did, it’s as if the care never happened.
How to Document:
- Be Detailed: Write clearly about the care provided and any changes in the patient’s condition.
- Include Quotes: If the patient or family member says something important, use quotation marks to note their exact words.
Additional Tips:
- Double-Check: Before leaving, make sure the bed is in the correct position and locked, and confirm that all documentation is complete.
- Consistency: Make these steps a routine part of your care process to ensure nothing is missed.

by editor | Feb 25, 2024 | Care Keys - Aides, Care Keys - Nurses, Care Keys - Social Workers, Keys to Compassionate Care, Patient Care, Teaching Tools
One of the greatest fears people face at the end of life is pain. Sadly, many individuals with serious illness still experience unnecessary suffering because pain is not fully recognized, effectively treated, or clearly communicated to the care team.
Pain affects more than just the body. It impacts emotional well-being, sleep, relationships, and peace of mind. When pain goes untreated or undertreated, patients may experience avoidable physical distress and mental suffering during what should be a time of comfort, dignity, and support.
Hospice care is uniquely focused on relieving pain and improving quality of life. Yet, many family caregivers struggle to assess their loved one’s discomfort or feel unsure about reporting changes. Common concerns include fear of medication side effects, worries about addiction, or uncertainty about when to request help. At the same time, patients themselves may underreport pain – sometimes to avoid “being a burden” or because they assume pain is inevitable.
The good news is that effective pain management is possible. It begins with understanding what matters most to the patient and communicating openly with the hospice team.
Foundations of Effective Pain Management
Respect the Patient’s Wishes
Every patient is unique. Their values, goals, and comfort preferences guide all pain-management decisions. Some patients wish to remain as alert as possible while others prioritize complete pain relief even if it causes increased sleepiness. Honoring these wishes ensures care remains both compassionate and personalized.
Consult and Involve the Patient
Whenever possible, pain-management choices are made in partnership with the patient. Listening to a patient’s concerns and preferences helps tailor medications and therapies to meet individual needs and care goals.
Collaborate as a Team
Hospice pain management is a team effort. Physicians, nurses, medical directors, social workers, chaplains, hospice aides, caregivers, and – most importantly – the patient work together to create and adjust a care plan that provides comfort and dignity. Communication among everyone involved ensures that changes are identified quickly and addressed effectively.
How Pain Is Managed and Monitored
Individualized Assessment
Pain treatment begins with careful, ongoing assessment. Hospice nurses regularly evaluate pain levels using verbal reports or behavioral cues (such as facial expressions or restlessness for those who can’t communicate). These assessments guide medication choices and adjustments to ensure relief is optimized over time.
Treat Pain Early
Addressing pain at the earliest signs prevents it from worsening and becoming harder to control. Early intervention supports better comfort and reduces unnecessary suffering.
Encourage Open Communication
Patients and caregivers should feel empowered to speak openly about pain, at any time. Even small changes matter. Honest communication ensures the care team can respond promptly and fine-tune treatment, as needed.
Start Low, Adjust Thoughtfully
Pain medication often begins at lower doses to preserve alertness and minimize side effects. Dosage is then adjusted – called titrationb – ased on the patient’s pain levels and the patient’s response to treatment. The goal is always to find the best balance between comfort and quality of life.
Many patients receive:
- A long-acting medication to maintain steady pain control
- A breakthrough medication for sudden or increased pain
Consistent and Timely Medication
Medications should be given on the prescribed schedule, even if pain seems controlled at the moment. Routine dosing prevents pain from returning and maintains steady comfort.
Use a Pain Log
Keeping a simple pain log can be incredibly helpful. Record:
- Pain levels
- What medication was given
- Dosage
- Time of administration
- Any changes or side effects
This information allows the hospice team to recognize patterns and make needed adjustments more quickly.
Monitor for Side Effects
Common medication side effects such as drowsiness, nausea, or constipation are carefully monitored. The hospice team works proactively to manage these effects so comfort isn’t compromised. Regular assessments ensure the overall well-being of the patient remains the primary focus.
A Holistic Approach to Comfort
Effective hospice care recognizes that pain is more than a physical experience. Emotional distress, anxiety, loneliness, and spiritual concerns can all intensify how pain is felt. For this reason, hospice embraces a holistic approach that supports the whole person – body, mind, and spirit.
Alongside carefully managed medications, patients may find comfort through soothing touch, gentle music, calming scents, guided relaxation, and meaningful spiritual or emotional support. These therapies can ease tension, promote a sense of peace, and help patients feel more grounded and comforted during this deeply personal time. By addressing both physical discomfort and emotional well-being, holistic care creates a more complete and compassionate pathway to relief.
This comprehensive approach ensures that patients are not treated as a collection of symptoms, but as whole individuals whose comfort, dignity, and peace matter profoundly.
Comfort Is Always the Priority
No one should suffer unnecessarily at the end of life. With open communication, expert guidance, and compassionate teamwork, pain can almost always be effectively managed. Hospice exists to ensure each patient receives comfort-focused care that honors their dignity, eases suffering, and supports families every step of the way.
Comfort is not a luxury. Comfort is a right as patients travel through their final journey. Every person deserves to experience peace, dignity, and compassionate support during this sacred time of life.
Where can you find out more?





