Japan has long been the global benchmark for longevity, particularly among women. Traditional explanations have often pointed to a healthy diet and specific cultural practices. However, a new study published in BMC Medicine (2026) suggests a more complex reality. By comparing the entire population over age 75 in Sweden with significant cohorts in Japan, researchers discovered that Japan’s mortality advantage is most pronounced among those already using long-term care (LTC) rather than in the healthy population.
Understanding the “Care Advantage”
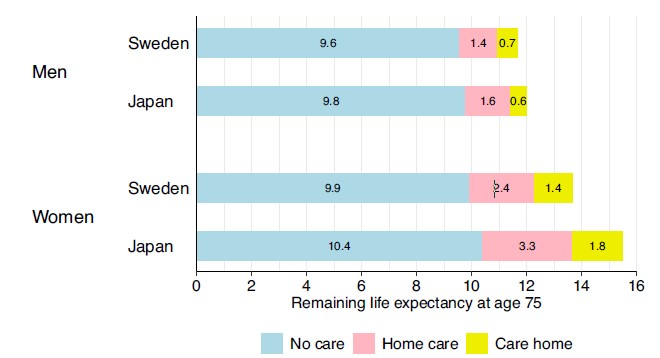
The study utilized a multistate model to track transitions between independent living, home care, and care home residence. Results showed that while a 75-year-old Japanese woman can expect to live 1.8 years longer than her Swedish counterpart, more than half of that extra time – roughly 1.3 years – is spent utilizing formal long-term care services. In fact, the mortality gap widened as the level of care increased: Japanese care home residents showed significantly lower death rates than those in Sweden, with differences reaching 148 deaths per 1,000 person-years for women.
Quality of Life vs. Quantity of Years
These findings indicate that Japan’s longevity may stem less from a “healthier” population and more from extensive, high-quality medical intervention and life-sustaining treatments within the LTC system. Japan is known for some of the most intensive medical care globally. This includes high rates of doctor consultations and longer hospital stays compared to Sweden. This “care advantage” suggests that the Japanese system excels at prolonging survival even after a person has become frail or severely disabled.
The Philosophical Crossroads: Life at Any Cost?
This data brings us to a profound ethical crossroads: what is the true goal of geriatric care?
If a significant portion of added life expectancy is spent in a state of high dependency, is our medical success occasionally clashing with the patient’s quality of life. In Japan, cultural values have historically emphasized extensive end-of-life care. Yet, this raises questions about whether we are prioritizing “life extension” over the dignity and autonomy of the individual.
Dignity in the “Dependent” Years
As we look to the future of hospice and palliative care, the Japan-Sweden comparison serves as a mirror for our own values. If the secret to longevity is more intensive medicalization of the elderly, are we prepared for the social and personal costs of prolonged frailty? Should public health success be measured by the number of years we can extract from a body? Or, should success be measured by alignment of medical care with a patient’s personal preferences and their sense of well-being in their final chapters.
Bridging the Gap in Hospice Care
Ultimately, the findings suggest that strategies to extend life must be balanced with the promotion of comfort and dignity. The challenge is ensuring that “more care” does not simply mean “more intervention.” Rather, additional care should be aligned with higher quality support that honors the human experience. We must continue to advocate for a care model where longevity never comes at the expense of a peaceful and dignified end-of-life journey.
Further Reading and References
- World Health Organization – Global Health Observatory Data (2024)
- OECD Health at a Glance 2025
- The Hastings Center – Ethics of End-of-Life Care
- International Association for Hospice & Palliative Care (IAHPC)
- Navigating Ethics in Hospice Care
- What Ethical Hospice Care Really Means at the End of Life
.
.
.
.




0 Comments